Group A Streptococcus (GAS) – also known as Streptococcus pyogenes – are bacteria which can colonise the throat, skin and anogenital tract.

In Scotland, GAS infection is monitored routinely using laboratory-confirmed positive specimen results. Laboratory confirmed infections from upper respiratory tract samples – for example, throat and nose samples – are considered a proxy estimate for cases of scarlet fever (which is not notifiable in Scotland).
GAS infection commonly presents as a mild illness with a sore throat. GAS can also cause a range of skin, soft tissue and respiratory tract infections.
In rare cases, people may go on to develop post-streptococcal complications, such as:
- rheumatic fever
- glomerulonephritis
GAS also can occasionally cause severe infections. Invasive GAS (iGAS) is an infection where the bacteria are isolated from a normally sterile body site, such as the blood.
Under the Public Health (Scotland) Act 2008, cases of iGAS are notifiable. iGAS cases are also reported to PHS through an enhanced questionnaire, which provides further information or risk factors and outcomes. In addition, invasive GAS samples are sent to the reference laboratory for further analysis and typing.
GAS is spread by close contact between people, through respiratory droplets and direct skin contact. It can also be transmitted environmentally, through contact with contaminated objects, such as towels or bedding or ingestion of food inoculated by a carrier.
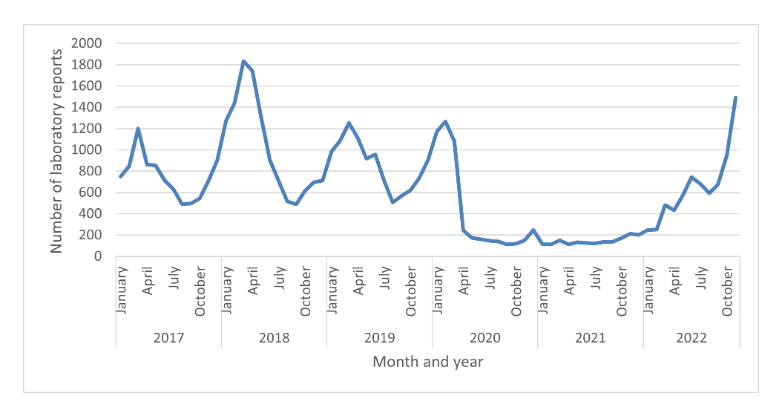
Currently, there is an increase in GAS in Scotland earlier in the season compared to recent seasons.
In the most recent time period (November 2022) there have been around 800 upper respiratory tract GAS (scarlet fever proxy) reports.
In the most recent time period (November 2022) there have been around 25 iGAS cases across all age groups. This compares with between 30 and 55 cases during peaks in previous years. Incidence is usually highest in those under the age of 10 years.
The next update from PHS: 14 December 2022
Click on this link for more information: NHS Inform Streptococcus A (strep A)
And this: UK Health Security Agency Group A Strep – What you need to know





Leave a Reply