It has been over a month since Scotland went into lockdown when the First Minster of Scotland called for an immediate stop to large public gatherings, citizens were asked to only shop for essential items and people were advised to socially isolate. All the measures have been on the whole adhered to by the public – no matter how hard they have been. On April 2nd Scotland stopped contact tracing .
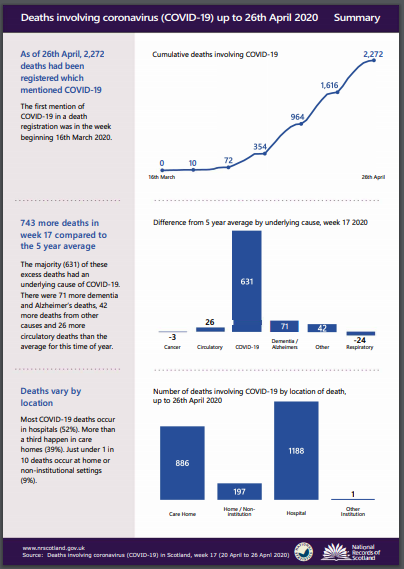
Since then Covid19 has ripped through our communities with the number of deaths reported by NRS (National Records of Scotland) in their weekly report climbing to 2,272 as of the 26th of April. This figure also includes the death of 11 health and care workers.
The number of deaths recorded in Scotland, on a weekly basis, is 68% more than would be normally recorded at this time of year.

Many care homes went into lockdown before the rest of Scotland but as you can see from the image the number of deaths in residential homes continues to rise – with the NRS weekly figures at 39% of all deaths but more recent statistics as stated by the First Minister Nicola Sturgeon on 29th of April , taking those figures to over half.
Professor Hugh Pennington
In his evidence to the Scottish Parliament’s Health and Sport Committee on 28th of April, Professor Sir Hugh Pennington of the University of Aberdeen expressed his view that the lockdown in Scotland had been successful. But went on to say:
“We do not have either a vaccine or antiviral drugs available for Covid-19, so prevention is paramount, and testing is the only way to know where the virus is.
“We have had a good test available since 13 January. Following the events in Wuhan, the Chinese did a genome sequence of the virus. That gave us information on which one could design a reverse transcription polymerase chain reaction—RT-PCR—test. Such tests have been around for a number of years, and many laboratories use the technique.”
Professor Pennington explained to the committee that despite there being a test available that all the facilities, including the international expertise of staff in biological research, was not being utilised.
On the ending of contact tracing by the Scottish Government on 2nd of April, Professor Pennington said:
” I do not know why the policy changed and why the idea of contact tracing was almost abandoned. My suspicion—although I do not have evidence for it—is that there was no testing capacity to do that. I think that the policy was driven by the lack of testing capacity, rather than the policy driving the need for more testing. That is my speculation.”
It is thought to be the case now that testing facilities are being underused although more will be known about that by the end of this week.
Professor Pennington also commented about the lack of appropriate PPE available and that staff should be trained in how to use it.
And he went on to say:
“In my view, social distancing is by far the most important aspect of the control measures that we put in place, followed by simple, straightforward things such as hand washing. The use of soap and water is extremely effective—I can quote the evidence in support of that if you would like me to. Those are the important things.
R Numbers
In his evidence to the Health and Sport Committee the question of R numbers also came up. These rate the level of transmission – and due to so little testing and no contact tracing it is extremely difficult to assess what the R number in Scotland might be. It is thought by the Scottish Government that it ranges between 0.6 and 1.
“If the R number is less than 1, it means that, on average, each person will infect less than one individual. If that is continued across the piece, the virus will die out, because it will eventually run out of people to infect. If the R number is greater than 1, the virus will continue to spread.” Prof Pennington
Professor Pennington suggested that in our care homes where Covid19 is ‘super spreading’ that the R number may be 10.
“That is based on the number of cases—the number of tragedies—in care homes. The number of people who have unfortunately died of Covid-19 is reported daily, and it will be an underestimate. We know that the virus does not cause 100 per cent mortality; even in high-risk groups, mortality rates are much less than that.
“The virus is going on the rampage in care homes.”
He explained to the MSPs that people going into care homes should be tested before being admitted. He went further and urged mass testing as the only way to prevent the spread of the virus.
“The more people we test, the better, but we should be looking at preventing the spread of the virus by stopping it from getting into care homes.
“We must make sure that no person, of any kind, who goes into a care home has the virus, because they might unwittingly spread it.
“It is not someone’s fault if they do not know that they have the virus. How could they know, when roughly 40 per cent of people who transmit it have no symptoms? People feel fine and go to work, so there has to be a testing regime to ensure that—as far as is humanly possible—the virus is not being carried into care homes, because of the risk of person-to-person spread.”
Could there be a different strategy for Orkney?
Professor Pennington also suggested that in Orkney there could be a different approach. Currently the numbers in Scotland are so high that contact tracing and testing would be extremely difficult. This is not the case in Orkney.
He said:
“Orkney, and the Western Isles are places where we could do something different from the rest of the country, because they have had very few cases and they have very good public health systems.
“They also have controls over incomers, in that people cannot go there unless they have a very good reason for going there.
“Those areas could come out of lockdown earlier: schools and small businesses could open, for example.
“That does not mean to say that it would be the end of the road in terms of the impact of the virus and the control measures, because no cruise liners would be welcome there and the fishing industry might have problems exporting fish and getting it to market outside the United Kingdom.”
Closing his evidence to the committee Professor Pennington said:
“I will just quote the director general of the World Health Organization, which is an organisation that I hold in high regard, despite what some folk have said. The director general said, “test, test, test”. If we can get that message across, get the testing really blasting away and get the facilities that exist in research units working night and day, we can sort this problem.”
And for people who are interested in how a country that took a different approach to the pandemic is faring, New Zealand has had to date a total of 19 deaths in comparison to Scotland’s 2,272.
And on Testing in New Zealand:-
“A high number of tests across the country helps identify cases of COVID-19 early, manage clusters of cases when we find them and track how well our efforts are working.This page records information about the ethnicity breakdown of testing and testing by region. It is updated weekly.
“Localised testing helps ensure we are both looking for and finding cases across the country.
“Surveillance testing – testing of a wider population to make sure there are not undetected cases – is also being carried out in parts of New Zealand.” Ministry of Health New Zealand
New Zealand has conducted to date 128, 703 tests ; Scotland 53,082 tests.
You can watch the Health and Sport Committee on 28th of April 2020 here
Reporter: Fiona Grahame





Leave a Reply