Continuing our series exploring Orkney’s current situation and possible future, we follow on from Exploring Orkney’s Constitutional Future: Education, with a look at
Health and Social Care.
Services in Orkney in Health, Social Care, Wellbeing etc are provided by a mixture of organisations: NHS Scotland; Council Social Care; Third Sector (national and local); private (dentistry); GP services; pharmacy which all work together in a complicated structure of provision which crosses over and interlinks with one another.
In Scotland, the NHS provides free care at point of need.
The Orkney Health and Social Care Partnership, (Orkney HSCP) is a partnership between Orkney Islands Council and NHS Orkney.
The Orkney HSCP has, to date, been responsible for the delivery of the full range of the Council’s social work and social services, for all age groups and service user groups, and NHS Orkney’s community based health services since 2011, under joint management arrangements. The Partnership has continued to be accountable to both the Council and NHS Orkney for the effective delivery of these services through the Board. Orkney Health and Social Care
It is a mammoth task to deliver the quality services we have in Orkney and the structure is currently under review as Scotland looks towards a developing a National Care Service
As part of Scotland , there is free personal care for those who require it which has been available since 2002. For those who ‘self-fund’ their residential care they receive an allowance in recognition of their personal and nursing care costs which has been raised in Scotland.
Scottish Statistics for the period 2020 – 21 are as follows:
Care Home Clients
- In 2020-21, there were 28,120 long-stay residents aged 65 and over in Care Homes in Scotland, 9% fewer than in 2011-12 and 8% fewer than in 2019-20, immediately before the COVID-19 pandemic
- In 2020-21 10,420 of these residents received FPNC (Free Personal Nursing Care) payments, 7% more than in 2011-12
- 6,870 self-funding Care Home residents aged 65 and over received both FPC and FNC payments in 2020-21
- 3,550 self-funding Care Home residents aged 65 and over received FPC payments only in 2020-21
Care at Home Clients
- In 2020-21, 49,780 people aged 65 and over received care at home. 46,820 of these people received personal care services at home.
- People aged 65 and over receiving personal care at home received an average of 9.8 hours per week of care in 2020-21
Care Home Expenditure
- FPNC payments to self-funding Care Home residents aged 65 and over are estimated to have cost Local Authorities £127 million in 2020-21 – an increase from £107 million in 2011-12, but a decrease from £142 million in 2019-20
Care at Home Expenditure
- Local Authorities spent £433 million on providing and purchasing personal care services for people aged 65 and over living at home in 2020-21 – representing a long-term increase from £347 million in 2011-12
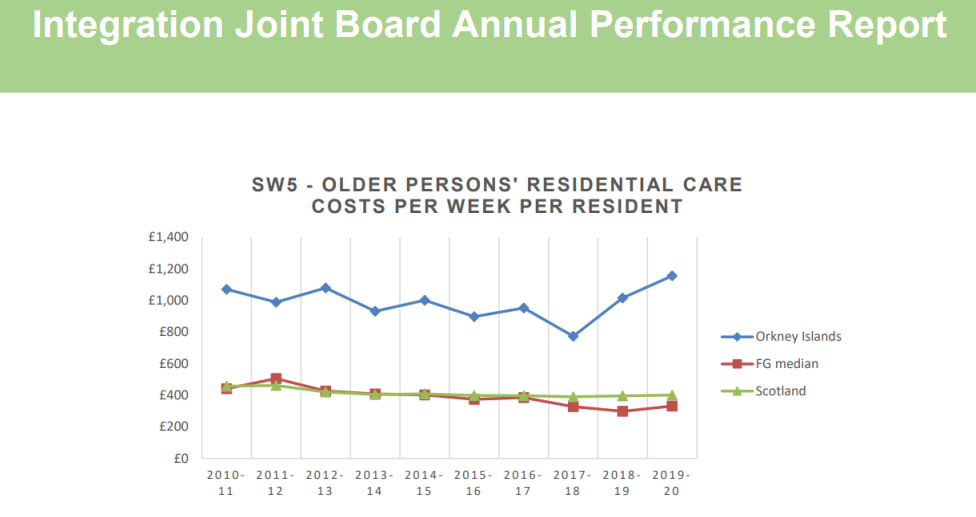
The Covid pandemic has had a huge impact , and continues to do so, on the cost and delivery of health and care services. The Annual Performance Report from Orkney’s joint Integration Board in 2020-21 states:
The impact of COVID-19 on services commissioned by the IJB has been unprecedented. It has required a significant degree of service change within a short period of time, ultimately having a substantial financial impact, which is likely to continue over the medium term

With an aging demographic the cost of these services in Orkney will continue to increase as more people require assistance to live in residential homes or independently in their own home .
Care Homes in Orkney, unlike most of Scotland, are managed by the local authority. Islanders will be aware of the building programme for Care Home facilities, for example A Look Around Hamnavoe House Care Home Stromness

As part of Scotland islanders receive: free NHS prescriptions, free eye & hearing tests, free dental checks and for those eligible free treatment. There are also the national screening programmes for early detection and preventative care such as the bowel screening kits sent out to homes, and breast and cervical screening, for example. The provision of these services was celebrated only last week when we remember that it has been 75 years since the founding of the NHS. Today Orkney has the new facilities offered at NHS Balfour Hospital.

The £65million hospital built by Robertson’s opened in 2019 and was Scotland’s first net zero hospital.
The Covid pandemic reminded us, if ever we need to be, of the magnificent health and social care services we have and of a workforce dedicated to the service. But recruitment is difficult, especially for islands, and Orkney is struggling to fill many posts. Those coming to Orkney to work also encounter difficulties finding affordable accommodation – something we will cover in a future article on Housing.
The work of the Third Sector in Orkney is outstanding and these organisations are often the first those with needs and concerns contact. All of these groups and organisations have been facing challenges around funding. Some are members of national bodies in Scotland and the UK, others are purely local. All are invaluable and often fill a gap that NHS Orkney and the council services cannot provide.
And no article on health and social care should ever miss out the unpaid carer – the backbone of the whole system.
“It is estimated by Carers UK that the value of the support provided by unpaid carers in Scotland is £10.8 billion each year, with 69 per cent of current Carer’s Allowance recipients women. In August 2021 there were around 81,400 carers in Scotland in receipt of Carer’s Allowance.”
Carer’s Allowance is the main benefit specifically for carers. It is paid at £69.70 per week. Most people in Scotland who receive Carer’s Allowance receive an automatic six-monthly payment of Carer’s Allowance Supplement from Social Security Scotland. From April 2022, the rate will be £237.90 per payment. The Carer’s Allowance Supplement is usually paid in June and December. Age Scotland
If Orkney was to separate from Scotland and the UK, the provision of Health and Social Care Services – the huge range that covers, including benefits, operations and medical care conducted outwith Orkney – all of that would require to be negotiated and funded.
So what could change if Orkney decides to separate from Scotland which it has been part of for over 550 years?
Some examples
The States of Guernsey, Crown Dependency, population over 63,000
The Committee for Health & Social Care provides some of the of health and social care services for the Bailiwick of Guernsey. Other providers are Primary Care, The Medical Specialist Group and Allied Health Professionals – these include Osteopaths, Psychologists & Art Therapists.
Guernsey is not part of the NHS, however, it has now reached agreement with the UK Government on a reciprocal health agreement between Guernsey and the British Government. This will enable residents from each jurisdiction to access medically necessary healthcare free of charge whilst they are visiting the other jurisdiction, if that treatment cannot wait until the individual returns to their home jurisdiction. Any UK residents requiring necessary healthcare whilst in the Islands of Guernsey must use a recognised provider, and should bring their GHIC/EHIC card with them. Travellers from the UK are still strongly advised to purchase travel insurance before travel, as the Arrangement does not cover everything that a person may end up needing whilst visiting (for example repatriation).
For visitors not from the UK: Primary care doctors, dentists and other health professionals, such as physiotherapists, are in private practice and all patients are required to pay for treatment. This can be at a surgery, at your temporary residence, or at the Princess Elizabeth Hospital including Accident & Emergency. There are also charges for the ambulance service and repatriation, to where you are ordinarily resident, if required. For visitors joining us from destinations other than the UK, medical insurance is strongly recommended – Health and Medical care in Guernsey
The Faroes, an autonomous territory of the Kingdom of Denmark. Population 54,000
The health care system is mainly based on publicly provided and financed services, as the private part is limited to e.g. dental care and physiotherapy.
The Chief Medical Officer is employed by the Danish Ministry of Health. The Chief Medical Officer shares responsibility with the Danish Board of Health for supervision of health services in the Faroe Islands.
Hospital services are run by the Home Rule Government which defrays all expenditure on operation and maintenance.
There are three local hospitals.
All practising physician are public employees, but they are mainly remunerated by the public health insurance scheme (Heilsutrygd). Physician services are administered by both the municipal authorities and the state authorities.
The midwife service is organized under the hospital services.
Pharmacies are run by the public authorities. – Healthcare in the Faroe Islands
The Faroes also conducts research into its health issues, one of which we covered in this archived piece from 2018: The Islands and the Whales
Norway, Independent Nation , population 5.4million
Norway’s healthcare is not free, but it is heavily subsidised. The Norwegian healthcare system is founded on the principles of universal access, decentralisation and free choice of provider. Healthcare in Norway
Norwegian expenditure on healthcare is the highest in the world. Every member of the Norwegian National Insurance scheme has the right to access healthcare services. Norwegians pay for the subsidised service at point of need and there is a limit on how much is paid.
The World Health Organisation describes it thus: “Norway’s health care system is universal, covering the whole population, and provides a broad range of services for residents. The health system is semi-decentralized, with four Regional Health Authorities (RHAs) being responsible for specialist care and municipalities responsible for primary care, long-term care and social services. “
Just a quick sample of some of the issues Orkney will have to consider if it takes the route put forward by the Leader and Depute Leader of OIC to separate from Scotland and the UK. The reorganisation of Health and Social Care services, the financing of them and reaching agreements on the provision of services not available in Orkney , including research, staffing and recruitment and benefit payments, all of these and more have huge implications for islanders to consider.
Fiona Grahame






Leave a Reply